IgG Food Allergy RESOURCES
Specimen Type: Serum or DBS
Turnaround Time: 1-2+ weeks
Test Markers: 190 foods plus Candida and Yeast
IgG Food MAP with xMAP® Technology
Now with Revolutionary Immunofluorescent Bead Technology
Assesses 190 Foods
Includes a wide range of foods, common in the Western, Asian, and Mediterranean diets. We have added a hemp allergy marker because it is very common now as a food source or as medical CBD. We are able to run the IgG Food MAP on both serum and dried blood spot samples.
Superior Sensitivity and Accuracy Compared to ELISA
GPL’s xMAP® immunoassay with fluorescence readout has proven to be even more sensitive than ELISA tests. The IgG Food MAP test detects all food antibodies with greater precision than ELISA tests thanks to the superior technology we've developed for the test.
Greater Reliability of Results
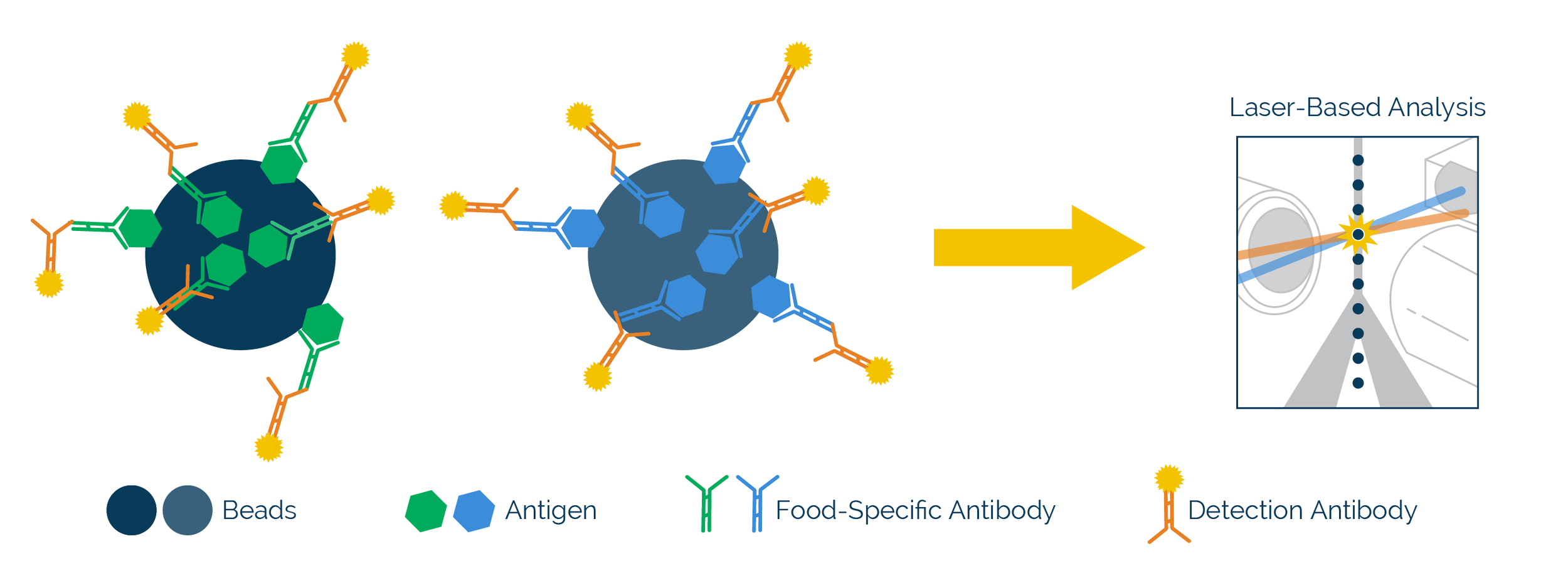
In the multiplexed bead-based immunoassay, food antigenic proteins are first covalently bound to beads. The beads are mixed with the patient’s sample where bead-bound antigens capture the specific IgG antibodies present in the sample. The food-specific IgG antibody level of each sample is detected with a fluorescent-labeled antibody against IgG. Every reaction with a patient sample also contains control beads to ensure accurate results. The fluorescent signal is measured using an xMAP® analyzer. The amount of food-specific antibody detected per allergen specific bead is directly proportional to the fluorescent signals. The higher the fluorescence, the more specific IgG antibodies are present in the sample. Once test results are available for review, our Quality Assurance (QA) team carefully verifies that quality control measures are within instrument and assay specifications.
Upgraded Technology
Antigen-specific IgG antibodies are captured on multiplexed magnetic beads, using xMAP® (Multiple Analyte Profiling) technology. The xMAP® bead-based immunoassay allows for the simultaneous detection of IgG antibodies to all 190 foods in two single test wells, reducing sample volume requirements and reagents while increasing sensitivity and specificity as compared to traditional plate-based ELISA tests. The upgraded immunoassay is cost and time effective, easy to perform and reproducible. We have now fully automated all steps of our testing processes, leading to even better precision.
Ecofriendly Technology
The xMAP® bead-based immunoassay is environmentally friendly, reducing plastic pollution. In the ELISA, a panel for 190 foods would require 190 wells (2 plates) per sample. In contrast, the beadbased platform only requires two wells per sample. In other words, the bead-based immunoassay would use just one plastic microtiter plate for testing 48 samples, while the ELISA would use 96 plates to test the same number of samples.
Tests for Specific Food Antigenic Proteins
GPL has upgraded from the ELISA’s single analyte detection to multiple analyte detection. The multiplexed, bead-based assay only detects IgGs against food antigenic proteins that were covalently bound to the beads, making this assay more specific to proteins than the ELISA. In the ELISA, there is no covalent binding of proteins; instead, proteins or other antigens are bound to the surface of a plastic well by adsorption. This non-specificity of the surface allows the binding of glycan-rich molecules such as Candida and yeast. Because of this, GPL is providing a separate report for the yeasts which will be tested by ELISA, rather than the xMAP® immunoassay.
What is IgG?
IgG is the major antibody found in serum. IgGs are composed of two fragment antigen binding (Fab) regions that contain the antigen binding sites and the Fc region, which is responsible for most of the biologic activity of the antibodies (Figure 1). An antigen is a substance that causes the immune system to produce an antibody that specifically reacts with it. IgG-mediated reactions to food antigens may be delayed by several hours or days, whereas IgE food antibody reactions are quite immediate.
Human IgG is separated into four subclasses denoted IgG1, IgG2, IgG3, and IgG4. Each subclass varies in abundance and biological function. IgG1 and IgG3 are predominantly responsible for antibody protection against reinfection. IgG2 antibodies are opsonic (marking a pathogen for ingestion and destruction) and develop in response to carbohydrate polysaccharide antigens. IgG4 molecules function as skin-sensitizing immunoglobulins and are thought to block antibodies produced in response to chronic exposure to antigens.
Why Test IgG Sensitivities?
Immunoglobulin G (IgG) food testing is a useful guide for structuring elimination diets for patients with many chronic conditions. Individuals with neurological, gastrointestinal, movement, and behavioral disorders often suffer from IgG food sensitivities. People may continue to eat offending foods unaware of their potential adverse effects. Symptoms associated with food sensitivities may occur hours or days after the offending food was eaten because IgG food antibodies remain for a much longer time than IgE antibodies. IgE food allergy causes the release of histamine, producing an immediate hypersensitivity reaction. In contrast, IgG food sensitivity is triggered by the binding of complement to IgG food antigen complexes, causing an inflammatory response. This is a delayed hypersensitivity reaction in which symptoms appear anywhere from hours to days after eating the offending food. Elimination of IgG-positive foods may improve symptoms of irritable bowel syndrome, autism, AD(H)D, cystic fibrosis, rheumatoid arthritis, and epilepsy, according to numerous clinical studies.
Clinical Significance of IgG Testing
The clinical significance of IgG food testing was illustrated in an early article published by an otolaryngologist who reported that the majority of his patients had substantial health improvements after eliminating foods found positive by IgG food allergy testing. The study demonstrated a 71% success rate for all symptoms, achieving at least a 75% relief. Of particular interest was the group of patients with chronic, disabling symptoms, unresponsive to other intensive treatments. Symptoms most commonly improved (75%-100%) on the elimination diets included asthma, coughing, ringing in the ears, chronic fatigue, headaches, gas, bloating, diarrhea, skin rash and itching, and nasal congestion. The most common IgG food allergies were to cow’s milk, garlic, mustard, egg yolk, tea, and chocolate. A recent study reported that 93% of non-celiac, gluten-sensitive patients showed anti-gliadin IgG antibody disappearance after a six-month adherence to a gluten-free diet. The IgG disappearance was closely related to a significant improvement of both gastrointestinal and extra-intestinal symptoms. High IgG antibody levels have frequently been found in children with diabetes mellitus, Crohn’s disease, celiac disease, and in those considered to be obese. IgG food test results are often used to develop food antibody-guided exclusion/ elimination diets. The implementation of such diets has been shown to alleviate symptoms associated with nonceliac gluten sensitivity and food sensitivity-induced atopic conditions, reduce the frequency of migraine headaches, decrease the occurrence of diarrhea, decrease failure–to-thrive among children with cystic fibrosis, reduce symptoms of irritable bowel syndrome, improve rectal compliance, decrease stool frequency in Crohn’s disease, prevent seizures and hyperkinetic behavior in children with epilepsy, and ameliorate kidney function in glomerulonephritis. Food elimination diets also hold promise for the improvement of behaviors associated with attention-deficit hyperactivity disorder.
Significance of Total IgG Versus IgG4
The goal of IgG-mediated food allergy testing is to identify foods that are capable of triggering many adverse reactions. IgG1, IgG2, and IgG3 are all capable of causing inflammation. IgG1, IgG2, and IgG3 antibodies to food antigens form large immune complexes or lattices that activate complement proteins and increase inflammation. IgG4 antibodies to food antigens will not usually trigger inflammation because IgG4 antibodies do not bind complement. However high levels of these antibodies indicate the presence of immune reactions against food antigens. Similarly IgA antibodies are not as clinically significant due to their inability to bind complement and trigger inflammation.
While most laboratories only provide a measurement of IgG4 molecules, The Great Plains Laboratory provides a measurement of total IgG antibodies to various food-based antigens and Candida, a genus of yeast native to the GI tract. Testing for only IgG4 antibodies limits the ability of the clinician to identify those foods that may be causing significant clinical reactions in their patients. IgG4 antibodies usually represent less than 6% of the total IgG antibodies. The importance of measuring all subtypes of IgG antibodies is highlighted in an article by Kemeny et al. They found that IgG1 antibodies to gluten were elevated in all patients with celiac disease but none of the patients had elevated IgG4 antibodies to gluten.
The IgG and Candida Connection
The Great Plains Laboratory tests for Candida albicans (a microscopic fungal organism and pathogenic yeast) as part of IgG food allergy testing. High levels of IgG antibodies to Candida have been found in patients who reported many symptoms of yeast overgrowth. Candida problems are caused when the benign yeast form of Candida albicans transforms to its fungal form and produces a buildup of toxins in the body. Candida can overgrow areas of the intestinal mucosa resulting in numerous symptoms, including creating microscopic holes in the lining of the intestines, leading to what is commonly known as “leaky gut” syndrome. Candida albicans proteins may trigger an inflammatory response. A wide range of disorders have been linked to Candida overgrowth including autism, multiple sclerosis, depression, chronic fatigue, fibromyalgia, migraines, and irritable bowel syndrome. Immunocompromised patients with cancer or AIDS can have life-threatening complications if Candida enters the bloodstream, resulting in systemic candidiasis. Use of antibiotics, oral contraceptives, chemotherapy, anti-inflammatory steroids, and diets high in sugar and starch increase susceptibility to Candida overgrowth.
Research has revealed a relationship between health of the gastrointestinal tract and overall well-being. Imbalance between good and bad bacteria (dysbiosis) has been shown to worsen behavior disorders, hyperactivity, aggression, and cause fatigue. Evidence is mounting that dysbiosis impairs the immune system and contributes to food allergies, digestive disorders, nutritional deficiencies, and cognitive dysfunction. Using the Food MAP (which will include a separate report for Candida and brewer’s yeast) will help identify food allergies and Candida sensitivity that may be creating a variety of problems for patients. Practitioners may then recommend elimination of the identified foods and supplementation with various natural products that control Candida overgrowth and assist with healing of the gut. Depending on the levels of Candida and the severity of a patient’s symptoms, further testing may be recommended, including a Comprehensive Stool Test or Organic Acids Test.
0-25th percentile: insignificant
26th-50th percentile: low
51st-97.5th percentile: moderate
97.5th and higher: high
THE BENEFITS OF TESTING
IgG testing determines if food reactions are contributing to physical or mental symptoms, and much more quickly than eliminating and then reintroducing each suspect food one-by-one over a period of time.
Removal of highly reactive foods from the diet is a non-invasive therapy that often mitigates a patient's symptoms.
Research and clinical studies suggest food allergies identified by IgG testing can be major contributing factors to many chronic health conditions.
Eliminating all identified IgG-positive foods after testing can reduce stress on the immune system, decrease inflammation (helping to heal “leaky gut”), resolve food cravings, and reduce the potential for eating disorders.
Multiple Analyte Profiling with xMAP® Technology
The bead-based immunofluorescent assay uses color-coded magnetic beads, which are covalently coupled to 190 different food proteins specific to each protein’s IgG target. The color-coding of the beads into spectrally distinct sets allows the simultaneous capture and detection of multiple food IgG analytes from a single reaction well.
The xMAP® bead-based immunoassay occurs on the surface of magnetic beads by adding a patient's serum sample and observing the classic antigen /antibody interaction, detected by using a fluorescent labeled antibody. Laser-based analysis of the fluorescent signal response is proportional to the binding of food-specific IgG antibodies onto the beads.
Analyte List (190 Foods + Candida & Saccharomyces Cerevisiae)
Dairy
Beta-Lactoglobulin
Casein
Cheddar Cheese
Cow's Milk
Goat's Milk
Mozzarella Cheese
Sheep's Yogurt
Whey
Yogurt
Beans and Peas
Adzuki Bean
Black Bean
Garbanzo Bean
Green Bean
Green Pea
Kidney Bean
Lentil
Lima Bean
Mung Bean
Navy Bean
Pinto Bean
Soybean
Tofu
Fruits
Acai Berry
Apple
Apricot
Banana
Blueberry
Cantaloupe
Cherry
Coconut
Cranberry
Date
Grape
Grapefruit
Guava
Jackfruit
Kiwi
Lemon
Lychee
Mango
Orange
Papaya
Passion Fruit
Peach
Pear
Pineapple
Plum
Pomegranate
Raspberry
Strawberry
Watermelon
Grains
Amaranth
Barley
Buckwheat
Corn
Gliadin
Malt
Millet
Oat
Quinoa
Rice
Rye
Sorghum
Teff
Wheat Gluten
Whole Wheat
Fish/Seafood
Abalone
Anchovy
Bass
Bonito
Codfish
Crab
Halibut
Lobster
Mackerel Saba
Octopus
Oyster
Pacific Mackerel (Saba)
Pacific Saury
Perch
Red Snapper
Salmon
Sardine
Scallop
Shrimp
Small Clam
Squid
Tilapia
Trout
Tuna
Meat/Fowl
Beef
Chicken
Duck
Egg White
Egg Yolk
Goose
Lamb
Pork
Turkey
Nuts/Seeds
Almond
Brazil Nut
Cashew
Chestnut
Chia Seed
Flax Seed
Hazelnut
Hemp Seed
Macadamia Nut
Peanut
Pecan
Pine Nut
Pistachio
Pumpkin Seed
Sesame Seed
Sunflower Seed
Walnut
Vegetables
Artichoke
Asparagus
Avocado
Bamboo Shoot
Bean Sprout
Beet
Bell Pepper
Bitter Gourd
Broccoli
Brussel Sprout
Burdock Root
Cabbage
Carrot
Cauliflower
Celery
Chili Pepper
Cucumber
Eggplant
Enoki Mushroom
Garlic
Kale
Leek
Lettuce
Lotus Root
Napa Cabbage
Olive (Green)
Onion
Portabella Mushroom
Potato
Pumpkin
Radish
Seaweed Kombu Kelp
Seaweed Nori
Seaweed Wakame
Shitake Mushroom
Spinach
Sweet Potato
Tomato
Yam
Yellow Squash
Yuca
Zucchini
Herbs/Spices
Basil
Bay Leaf
Black Pepper
Cayenne Pepper
Cilantro
Cinnamon
Cloves
Cumin
Curry
Dill
Ginger
Hops
Mint
Miso
Mustard Seed
Oregano
Paprika
Rosemary
Sage
Tarragon
Thyme
Turmeric
Vanilla Bean
Miscellaneous
Bromelain
Cane Sugar
Cocoa Bean
Coffee
Green Tea
Honey
Meat glue
Oolong Tea
SPECIMEN REQUIREMENTS
The IgG Food Allergy Test is available as both Serum and Dried Blood Spot.
Serum: 1 mL of in a gold-topped SST or in a royal blue-topped no additive tube.
Dried Blood Spot (DBS): Five full circles of dried blood on the protein saver card is required.
Please note that the elimination of a food prior to sampling will reduce the ability for our laboratory to detect antibodies (allergies) to that food.
Please note that the elimination diet is based only on IgG testing. To be safe, testing for IgE antibodies to food allergens should be considered PRIOR TO BEGINNING an ELIMINATION DIET. If a patient has negative results for IgG antibodies, it does not necessarily mean he/she is negative for IgE, IgM, or IgA antibodies.
TESTIMONIALS
"I believe the Great Plains IgG Food Allergy Test is a phenomenal tool that I have implemented in my practice on a daily basis to help treat patients for a wide variety of symptoms like headaches, IBS, fatigue, abdominal pain, dermatitis, hair loss, joint pain, acne, thyroid disorders, and vitamin deficiencies. I believe I am a better physician due to this testing transforming my ability to properly diagnose and treat patients effectively."
–Bridget, M.D.
References
Anderson S, Wakeley P, Wibberley G, et al. Development and evaluation of a Luminex multiplex serology assay to detect antibodies to bovine herpes virus 1, parainfluenza 3 virus, bovine viral diarrhoea virus, and bovine respiratory syncytial virus, with comparison to existing ELISA detection methods. J Immunol Methods 2011;366:79-88.
Gimenez-Lirola LG, Jiang Y-H, Sun D, et al. Simultaneous Detection of Antibodies against Apx Toxins ApxI, ApxII, ApxIII, and ApxIV in Pigs with Known and Unknown Actinobacillus pleuropneumoniae Exposure Using a Multiplexing Liquid Array Platform. Clin Vaccine Immunol 2014;21(1):85-95.
Langenhorst RJ, Lawson S, Kittawornrat A, et al. Development of a fluorescent microsphere immunoassay for detection of antibodies against porcine reproductive and respiratory syndrome virus using oral fluid samples as an alternative to serum-based assays. Clin Vaccine Immunol 2012;19(2):180-9.
Smits GP, van Gageldonk PG, Schouls LM, et al. Development of a Bead- Based Multiplex Immunoassay for Simultaneous Quantitative Detection of IgG Serum Antibodies against Measles, Mumps, Rubella, and Varicella- Zoster Virus. Clin Vaccine Immunol 2012;19(3):396-400.
Alpay, K. et al. Diet restriction in migraine, based on IgG against foods: a clinical double-blind, randomised, cross-over trial. Cephalalgia : an international journal of headache 30, 829-837, doi:10.1177/0333102410361404 (2010).
Mitchell, N. et al. Randomised controlled trial of food elimination diet based on IgG antibodies for the prevention of migraine like headaches. Nutrition journal 10, 85, doi:10.1186/1475-2891-10-85 (2011).
Zar, S., Mincher, L., Benson, M. J. & Kumar, D. Food-specific IgG4 antibody- guided exclusion diet improves symptoms and rectal compliance in irritable bowel syndrome. Scandinavian journal of gastroenterology 40, 800-807, doi:10.1080/00365520510015593 (2005).
Atkinson, W., Sheldon, T. A., Shaath, N. & Whorwell, P. J. Food elimination based on IgG antibodies in irritable bowel syndrome: a randomised controlled trial. Gut 53, 1459-1464, doi:10.1136/gut.2003.037697 (2004).
Drisko, J., Bischoff, B., Hall, M. & McCallum, R. Treating irritable bowel syndrome with a food elimination diet followed by food challenge and probiotics. Journal of the American College of Nutrition 25, 514-522 (2006).
Bentz, S. et al. Clinical relevance of IgG antibodies against food antigens in Crohn’s disease: a double-blind cross-over diet intervention study. Digestion 81, 252-264, doi:10.1159/000264649 (2010).
Egger, J., Carter, C. M., Soothill, J. F. & Wilson, J. Oligoantigenic diet treatment of children with epilepsy and migraine. The Journal of pediatrics 114, 51-58 (1989).
Pelsser, L. M. et al. Effects of a restricted elimination diet on the behavior of children with attention-deficit hyperactivity disorder (INCA study): a randomized controlled trial. Lancet 377, 494-503, doi:10.1016/S0140- 6736(10)62227-1 (2011). 8b cookbook
Veling, M. & Trevino, R. (2002). Food allergies and hypersensitivities. Alexandria, VA: American Academy of Otolaryngology-Head and Neck Surgery Foundation.
Dixon H, Treatment of delayed food allergy based on specific immunoglobulin G RAST testing relief. Otoloryngol Head Neck Surg 2000;123:48- 54.
Ciao, G. et al, Effect of gluten free diet on immune response to gliadin in patients with non-celiac gluten sensitivity. BMC Gastroenterology 14, 26 (2014)
Kemeny DM, et al Sub-class of IgG in allergic disease. I. IgG sub-class antibodies in immediate and non-immediate food allergy. Clin Allergy. 1986; 16:571-81
Hofman, T. IgE and IgG antibodies in children with food allergy. Rocz Akad Med Bialymst 40, 468-473 (1995).
Jenmalm, M. C. & Bjorksten, B. Cord blood levels of immunoglobulin G subclass antibodies to food and inhalant allergens in relation to maternal atopy and the development of atopic disease during the first 8 years of life. Clinical and experimental allergy : journal of the British Society for Allergy and Clinical Immunology 30, 34-40 (2000).
Lucarelli, S. et al. Food allergy in cystic fibrosis. Minerva pediatrica 46, 543-548 (1994).
van der Woude, F. J. et al. Do food antigens play a role in the pathogenesis of some cases of human glomerulonephritis? Clinical and experimental immunology 51, 587-594 (1983).
James L.K and Till S.J Potential mechanisms for IgG4 inhibition of immediate hypersensitivity reactions. Current Allergy Asthma Rep. 16:23, 2016 PMID: 26892721
Caubet J.C. et al. Natural tolerance development in cow’s milk allergic children: IgE and IgG4 epitope binding. European Journal of Allergy and Clinical Immunology, First published: 27 March 2017
THIS TEST IS ALSO KNOWN AS:
PRUEBA DE ALERGIA IGG FOOD + CÁNDIDA
IGG食物アレルギー検査+カンジダ
تحليل حساسية أغذية + فطر الكانديدا
IGG NAHRUNGSMITTELALLERGIE-TEST + CANDIDA
IGG ALLERGIE ALIMENTAIRE ESSAI + CANDIDA
IGG CIBO PROVA DI ALLERGIA + CANDIDA
IGG의 식품 알레르기 테스트 + 칸디다
IGG FOOD TEST NA ALERGIĘ + CANDIDA
TESTE DE ALERGIA IGG FOOD + CANDIDA
IGG GIDA ALERJISI TESTI + CANDIDA
IGG的食物过敏测试+念珠菌